On-Demand Outsourcing BPO Services for Healthcare Providers With 24/7 Coverage!
Save up to 70% on staffing costs!
Browse Specialty Staffing Services
Why do specialty medications hit a bottleneck in the prior authorization process?
A provider prescribes a life-changing specialty medication. The patient is ready to begin treatment. But as days turn into weeks, hope is replaced by frustration. Behind the scenes, staff scramble to meet payer demands faxing paperwork, calling support lines, chasing clarifications. The medication isn’t the problem. The prior authorization (PA) process is. Unfortunately, this is not an isolated case. It’s a daily obstacle for clinics navigating high-stakes prescriptions through outdated, high-friction systems. What Is Prior Authorization? Prior authorization is the

How to Optimize Coding for Specialty Medications in Revenue Cycle Management?
Specialty medications are crucial in treating complex conditions like cancer, rheumatoid arthritis, and multiple sclerosis. However, their unique characteristics — high costs, complex administration methods, and the need for precise billing codes — make them one of the more challenging aspects of healthcare revenue cycle management (RCM). In this article, we’ll delve into how optimizing coding for specialty medications can improve reimbursement accuracy, minimize denials, and streamline the RCM process for healthcare providers. Key Takeaways Accurate coding for specialty medications

What Are the Key Benefits of Outsourcing LTC Pharmacy Billing?
Long-term care (LTC) pharmacies face unique challenges when it comes to billing and reimbursement. With patients who require ongoing, specialized care, accurate and timely billing becomes crucial for the financial health of these pharmacies. Navigating complex medication regimens, coordinating with multiple insurance plans, and ensuring proper documentation can be overwhelming. However, outsourcing LTC billing services to experts like Staffingly, Inc. can streamline these processes, reduce errors, and ensure that pharmacies get reimbursed quickly and accurately. By prioritizing outsourced billing services

How Can Outsourcing Help Solve Specialty Medication Billing Challenges?
Billing for specialty medications is much more complex than billing for standard prescriptions. These medications often come with high costs, require extensive prior authorization, and involve unique payer rules that vary widely across insurance plans. As a result, healthcare providers and pharmacies managing specialty drugs face several challenges, including delayed reimbursements, denied claims, and significant administrative burdens. However, outsourcing billing for specialty medications can be a game-changer. By leveraging external expertise, providers can navigate these complexities more effectively. Furthermore, outsourcing

How Does Specialty Pharmacy Service Outsourcing Enhance Complex Treatment Patient Care?
As healthcare providers, we know firsthand how critical it is to manage complex treatments for patients with chronic or rare conditions. Whether it’s ensuring timely access to life-saving medications, coordinating prior authorizations, or managing side effects, specialty pharmacy services often require resources that stretch even the most capable teams. For many clinics, hospitals, and private practices, juggling these responsibilities while maintaining a high level of patient care can feel overwhelming. Outsourcing specialty pharmacy services has become a game-changer in this
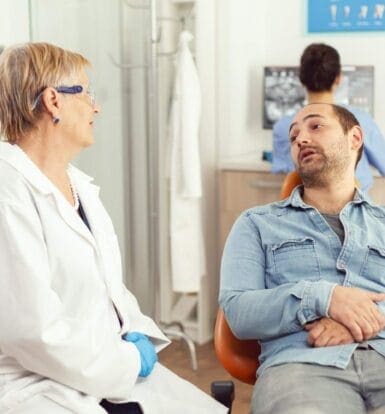
Step-by-Step Guide to Epclusa Prior Authorization
If you’ve ever had to handle insurance prior authorization, you know how daunting it can feel—especially for high-cost medications like Epclusa (sofosbuvir/velpatasvir). Whether you’re a healthcare provider, pharmacist, or patient advocate, the process can often seem like a mountain of paperwork, phone calls, and delays. But here’s the thing—it doesn’t have to be overwhelming. With the right information and a clear plan, navigating prior authorization for Epclusa can be manageable and even straightforward. In this guide, we’ll go step by

How Outsourcing Specialty Pharmacy Services Improves Patient Care?
If you’re a healthcare provider working with complex treatment plans, you’ve likely encountered the challenges that come with managing specialty pharmacy services. Between navigating prior authorizations, coordinating with insurance companies, and ensuring patients receive their medications on time, the process can feel overwhelming. And when you’re juggling these responsibilities alongside direct patient care, something is bound to give. Outsourcing specialty pharmacy services has emerged as a practical, effective solution for healthcare providers looking to balance these demands. By handing off

Steps to Obtain Prior Authorization for Sevelamer in CKD
Healthcare providers often face challenges in navigating the prior authorization (PA) process, especially when dealing with patients with unique needs like difficulty swallowing. Phosphate binders play a crucial role in managing phosphate levels, especially for patients on dialysis or with advanced CKD. Medications like Sevelamer Carbonate are often prescribed to manage these levels, especially when patients struggle with swallowing standard pills or tablets. Sevelamer Carbonate is a specialty drug that requires prior authorization due to its specific indications and cost.
 Book a Demo to Build Your Team Today!
Book a Demo to Build Your Team Today!


 Read Case Studies
Read Case Studies 



 Virtual Medical Assistants
Virtual Medical Assistants



