On-Demand Outsourcing BPO Services for Healthcare Providers With 24/7 Coverage!
Save up to 70% on staffing costs!
Browse Specialty Staffing Services
How to Get Caremark’s Prior Authorization for Air Suppress Aerosol for Severe COPD?
Introduction Imagine you’re working with a patient who has chronic obstructive pulmonary disease (COPD), and despite trying multiple medications, they’re still struggling to control their severe respiratory symptoms. Standard inhalers aren’t providing the relief they need, and after some trial and error, Air Suppress 9280mcg Aerosol has finally made a difference, helping them breathe easier and improve their quality of life. However, because Air Suppress isn’t on Caremark’s standard formulary, you’ll need to secure prior authorization (PA) to ensure the

What’s the Process for Sevelamer Prior Authorization in CKD?
In healthcare, obtaining insurance prior authorization (PA) for essential medications can be a bit of a journey, especially when it comes to specialized treatments. This guide walks through a recent case of securing PA for Sevelamer Carbonate, a crucial medication for managing chronic kidney disease (CKD). Used to help reduce high phosphate levels in CKD patients, Sevelamer is an effective solution but often comes with the challenge of needing prior approval from insurance companies. Let’s look at how we navigated

How Do You Get Prior Authorization for Oxycodone 30MG?
Managing prior authorization (PA) for controlled medications like Oxycodone requires precision and a patient-focused approach. I’ll walk you through the process to secure PA for Oxycodone 30MG tablets with Optum RX. This can be especially helpful for healthcare providers and insurance specialists alike, as understanding each step makes the process smoother and helps patients access the necessary pain relief they deserve while staying compliant with stringent guidelines. Insurance Company Overview Optum RX, a leading pharmacy benefits manager, supports millions with
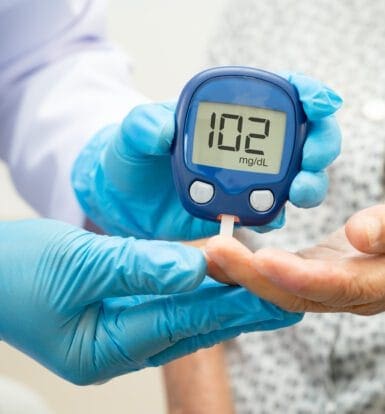
How Can I Get Prior Authorization for Novolog for Diabetes?
Getting prior authorization (PA) for Novolog, a fast-acting insulin, is a detailed process, especially for Type 2 diabetes patients who require insulin via an infusion pump. This case highlights how to work through an insurer’s requirements to ensure the medication approval process is as seamless as possible. We’ll break down the steps we took, key points we clarified, and insights on how using Staffingly Inc.’s services can smooth this process for healthcare providers. Insurance Company Overview In this case, we’re

How Do You Get Insurance Approval for Ondansetron for Nausea?
If you’re managing prior authorization (PA) requests for a medication like Ondansetron to treat severe nausea and vomiting, you know it requires a step-by-step approach. In this case, we’ll explore a real-life PA request through Caremark Medicare, detailing each phase of the submission process and highlighting essential takeaways to help you ensure a smooth and successful request. Insurance Company and Medication Overview For this case, the PA request was processed with Caremark Medicare. They handle prior authorizations with a specific

How Do You Get Insurance Approval for Hydroxyzine for Anxiety?
When it comes to managing anxiety, medications like Hydroxyzine can provide essential relief, especially when traditional treatments fall short. However, obtaining insurance prior authorization (PA) for Hydroxyzine can be a complex process, especially as insurers carefully evaluate the need for medications with known risks or limited indications. In this step-by-step guide, we’ll walk through a real-world example of obtaining prior authorization for Hydroxyzine, highlighting the nuances and strategies that can make this process as seamless as possible. Insurance Company and

What’s the Process for Getting Insurance Approval for Formoterol?
When you’re working with a patient who has COPD, finding the right treatment is essential. Formoterol, a long-acting bronchodilator, is often prescribed to improve breathing and manage the symptoms of COPD. However, like many specialized medications, it frequently requires prior authorization (PA) to ensure insurance coverage. Today, let’s walk through the key steps and insights from a case where we successfully navigated a prior authorization request for Formoterol with UPMC Medicaid. This case will help you understand the essentials of

How Can You Get Propranolol Approved for Hypertension Treatment Through Prior Authorization?
Securing a prior authorization (PA) for essential medications like Propranolol, especially for chronic conditions such as hypertension, can be a nuanced and thorough process. It requires demonstrating the medical necessity of the medication while addressing insurers’ questions and gathering extensive documentation. In a recent case, I helped a patient receive Propranolol, a medication crucial to their blood pressure stability, by following a detailed PA approach. Let’s walk through how I tackled each step, from gathering documents to effectively presenting the
 Book a Demo to Build Your Team Today!
Book a Demo to Build Your Team Today!


 Read Case Studies
Read Case Studies 



 Virtual Medical Assistants
Virtual Medical Assistants



