On-Demand Outsourcing BPO Services for Healthcare Providers With 24/7 Coverage!
Save up to 70% on staffing costs!
Browse Specialty Staffing Services
Prior Authorization Support for Orthopedic and Pain Management Clinics
In orthopedic and pain management clinics, Prior Authorization is a necessary but often frustrating process. Insurance companies require approvals for procedures like joint replacements, spinal injections, and pain management medications, leading to administrative bottlenecks, delayed treatments, and revenue loss. With AI in telemedicine technology, Prior Authorization support is becoming more efficient, reducing wait times, minimizing denials, and improving the patient experience. Why Prior Authorization is Challenging for Orthopedic and Pain Management Clinics High Volume of Required Authorizations Orthopedic and pain

Steps for OxyContin Prior Authorization with Optum RX
Healthcare providers treating severe chronic pain often use OxyContin 10mg ER for relief. However, insurance providers like Optum RX Medicare Part D require prior authorization (PA) for opioid prescriptions. This step confirms the necessity of opioids and the exploration of alternative therapies. This guide outlines the process of obtaining PA for OxyContin, including documentation of past treatments and supporting documentation. Following these steps can streamline the process and prevent delays in patient pain management. Key Takeaways Optum RX Medicare Part
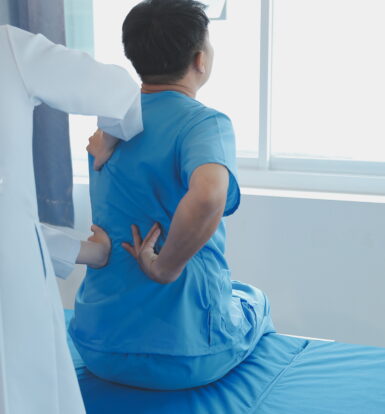
How to Get Prior Authorization for Hydromorphone with Optum RX Medicaid?
For patients with chronic pain, finding an effective treatment can be a long, frustrating journey. When common pain relief options don’t work, more potent medications like Hydromorphone HCL 2mg may be necessary. However, because Hydromorphone is a powerful opioid, Optum RX Medicaid requires prior authorization (PA) to ensure it’s being prescribed safely and only when truly needed. This extra step is designed to verify that other pain management options have been tried and were unsuccessful, and that Hydromorphone is appropriate

How Do You Get Prior Authorization for Oxycodone 30MG?
Managing prior authorization (PA) for controlled medications like Oxycodone requires precision and a patient-focused approach. I’ll walk you through the process to secure PA for Oxycodone 30MG tablets with Optum RX. This can be especially helpful for healthcare providers and insurance specialists alike, as understanding each step makes the process smoother and helps patients access the necessary pain relief they deserve while staying compliant with stringent guidelines. Insurance Company Overview Optum RX, a leading pharmacy benefits manager, supports millions with
 Book a Demo to Build Your Team Today!
Book a Demo to Build Your Team Today!


 Read Case Studies
Read Case Studies 


 Virtual Medical Assistants
Virtual Medical Assistants



