
Author: T.KATHYAYINI, ASN PHARMACY COLLEGE
CLINICAL PHARMACIST: Pharmacist is the bridge between doctors and patients who counsels and advice the patient to maximize the desired effect of the drugs and minimize the adverse effects of the drug.
The basic duty of a pharmacist is to check prescriptions from physicians before dispensing the medication to the patients to ensure that the patients don’t receive the wrong drugs or take an incorrect dose of medicine. Dispensing the wrong drugs or giving incorrect usage instructions can have serious consequences for patients, including death. Pharmacists also offer guidance on the side effects; medication can have and warn against actions that could be dangerous while the patient is using the medicine, such as consuming alcohol or operating heavy machinery.

ROLE OF CLINICAL PHARMACIST:
Pharmacist should always associate as a team member of health care professionals. Pharmacist is an expert person in decision-making process in matters of dosage regimens, monitoring of adverse drug reactions, interactions with medications, and interpretation of prescriptions as well as associated with drug and poison information services.
- Pharmacist has great role in the enrichment of treatment accuracy and uses several pharmaceutical services considering the patient safety and efficacy of
- Pharmacist is a qualified person in a hospital and should participate with team to promote healthcare practice in the management of
- Pharmacist should prevent negative perspectives of therapeutic outcome due to the medication errors and incorporation of incorrect dosage regimen.
RESPONSIBILITIES OF CLINICAL PHARMACIST:
Pharmacist should participate with physicians, he should do visit alone to provide information related with medication and its administration and necessary care to concerned patient.
- Pharmacist should follow the treatment given by the physician as well as check the prescribed dose by referring the
- Pharmacist may also think on the prescribed medication and assess the possible risk to the patients while drug administration and will report or alert to the health care team to prevent further
- Pharmacist should also motivate the patient while discharging regarding to take proper diet and exercise for disease management
THE RELATIONSHIP OF TRAID
CLINICAL REVIEW:
Clinical review is a system review or relevant information of all examination done by clinical pharmacist on response and monitoring of drug treatment and safety aspect on daily basis. The main approach of clinical review is to assess the therapeutic outcome of the dosage regimen and its safety. It is one of the integral parts of the medication chart review.
GOALS OF CLINICAL REVIEW:
Following are the primary goals of the clinical review:
- Evaluate the response and safety of drug
- Assess the improvement in the patient condition and the need to change in drug
- Evaluate the need of the therapeutic drug
- Check for patient compliance to
CRITERIA FOR EFFECTIVE PHARMACIST CLINICAL REVIEW:
Pharmacists have expertise and advanced training in the effective and appropriate use of medications. Following are some important criteria for effective clinical review:
- Ensure adequate training given to persons involved in clinical
- Main the good working relationship with all practitioners, other health care staff to permit clinical review of patient, assess clinical report and for effective
- Identify the expert to discuss any problems and
- Implementation systematic approach for the clinical review and always involve patient in
- Decide most reliable therapeutic intervention for the individual
- Before any recommendation to patient or practitioners, pharmacist must see the medical notes for any sensible issues related to
For example: pharmacist run anticoagulant clinics
Many pharmacist run anticoagulant clinics in developed countries. In their clinics, they estimate international normalized ratio (INR) for the patients who are an anticoagulant therapy. If INR is found more than normal, the dose of the patient is altered and if situation demands, the pharmacist may discuss the report with the patients G.P. for necessary treatment corrections.
MEDICATION REVIEW:
“Medication review is a structured evaluation of a patient’s medicines with the aim of optimizing medicines use and improving health outcomes. This entails detecting drug-related problems and recommending interventions”.
Medication review services are fast becoming popular in many countries, and are known for giving pharmacists basic knowledge as well as a practical exercise in delivering an additional service to their patients. Pharmacists who have successfully completed a follow-up or continuing education course may offer these services.

MEDICATION REVIEW PROCESS:
To evaluate the successes and barriers of the implementation of a pharmacist-led full medication review process in hospitals. The process consisted of three steps:
- Medication reconciliation upon admission;
- Medication review using an explicit reviewing tool followed by a discussion between the pharmacist and the doctor; and
- Medication reconciliation upon
The difference between the medical reconciliation and medication review are given below:
- Medication reconciliation: A goal of medication reconciliation is to create an updated list of medications that is maintained and guides therapy for the patient. Numerous studies have been published over the past two decades that have examined pharmacists’ role during the medication reconciliation process.
- Medicaion review: A medication review starts with establishing a best-possible medication history, and includes a critical evaluation of the patient’s medications for any potential drug-related issues (e.g. medications that may be necessary or unnecessary, drug interactions, ADRs, inappropriate dosing). Medication review often results in recommendations to change, discontinue or even start new medications.
The Institute for Safe Medication Practices Canada (ISMP) states that: “Medication reconciliation is intended to prevent medication errors at transition points in patient care, whereas medication review is intended to address drug-related problems arising over time.”
MEDICATION CHART REVIEW:
Medication chart review (MCR) is a fundamental responsibility of pharmacist to ensure appropriate medication order. The main objective of MCR are to optimizing the drug therapy, improving the health outcomes and reduce the medical related problems like untreated indications, inappropriate drug selection, drug interaction, overdose of any medication; and any errors that may occurs while prescribing of drug therapy and administration.
If the pharmacist found any errors or problem in medication chart then should write annotations on the chart at appropriate place where medication order is unclear.
- Pharmacist should check the medication order is written as per legal and local requirements also ensure the order is understandable and used appropriate name of the Pharmacist may also review the order for cost effectiveness of medication. If there is error observed in order then mark should be provided for clarification.
- Make sure that the medication order is correct with respect to previous order, specific condition of the patient (such as disease state, gender, pregnancy, age), dose and dosage schedules with considering of the patient conditions, dosage form and route and method of medication
- Pharmacist must check the order for duplication of medication, drug interaction as well as time of drug administration with respect to food and along with another
- Check whether there requires appropriate follow up for any medication or therapy monitoring is recommended in given
MEDICATION HISTORY:
Details information about medication history in terms of questions asked by pharmacist while interviewing the patients, type of information recorded in medical history.
Patient medication history provides the valuable information on the patient’s allergic tendency, patient compliance and self- medication. Such type of information of medication history helps the pharmacist to establish with patient, commencing of patient counseling and designing of pharmaceutical care plan.
PHARMACIST INTERVENTION:
Pharmacist intervention covers wide range of medication related issues. There is a necessary of pharmacist intervention to detect any problem with the medication therapy. In patient care services, there recognizes various untreated health issues and this can be resolved by choosing appropriate therapeutic regimen. Pharmacists follow the progress of therapeutic outcome.
Pharmacist involved in the review of prescription and if needed suggest the appropriate therapeutic regimen to improve the safety, efficacy as well as cost of medications. Method of pharmacist intervention considered has great inputs in the patient care system. In this, pharmacist role is to reduce the medication errors, justifying the use of therapeutic regimen in particular patient and reducing the cost of medications.
There have diversified role of pharmacist including the dispensing of medication, patient monitoring, patient counseling, health education, community services and clinical practices. It is recommended that all the prescription must be reviewed by the pharmacist before dispensing of medication to avoid the medication errors.
Importance of pharmacist intervention:
Medication errors may cause the consequences which may range from minor to seriousness and sometimes may require hospitalization or death of patient. Pharmacist intervention may reduce to this happen. Following are some objectives of pharmacist intervention.
- To review the prescription order before dispensing of the
- To prevent the development of complication and
- To improve the patient
- To reduce the cost and to improve the safety and effectiveness of
PHARMACEUTICAL CARE:
Pharmaceutical care is a practice of pharmacist to contribute to optimize the rational therapy towards improvement in the health status of patients. The major goal and output of the pharmaceutical care are, elimination or prevention of the disease symptoms, cure or slowing of disease condition.
The pharmaceutical care plan is prepared on the basis of clearly defined therapeutic goal. The pharmaceutical care plan is made in the form of written, individualized and comprehensive medication therapy. The responsibility of pharmaceutical care plan is delivered to pharmacists who are involved in direct patient care and is updated with each major change in patient status.
Functions of pharmaceutical care plan:
Following are the three main functions of pharmaceutical care plan:
- Identification of actual and potential drug- related problems in
- Resolve the patient’s actual drug- related
- Prevention of the patient’s potential drug- related
For example, the outcomes associated with pharmacist involvement in diabetes care in all pharmacy practice settings.
A total of 120 patients consented to participate in this randomized control study (fig. 1). Of the 120 patients, 20 patients were excluded. In the intervention group, 39 patients completed the eight visits with the pharmacists. On the other hand, 37 patients in the non-intervention group completed this study. The study observed the changes of glycaemic control, body mass index (BMI) and blood pressure within and between groups. The changes of lipid profile and adherence were only analyzed in intervention group as there was not sufficient data in non-intervention group. There were no differences of baseline HbA1c and FBG between groups.
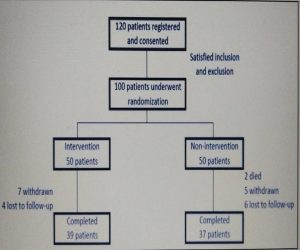
FIG: 1 Enrollment Randomization control study
The mean HbA1c in the intervention group decreased significantly. However, the reduction of mean HbA1c in the non-intervention group was not significant. The mean HbA1c reduction of in the intervention group was significantly different than the reduction in the nonintervention group. Sixteen patients had significantly achieved at least 1% drop in HbA1c in the intervention group as compared to eight patients in the non-intervention group (fig. 2).
In addition, the FBG was significantly improved in the intervention group with a reduction and there was significant difference of mean FBG between the intervention and non-intervention groups
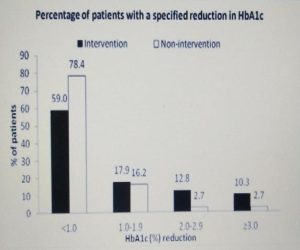
FIG: 2 Percentage of patients with a specified reduction in HbA1c
The difference of systolic blood pressure was significant between groups with the reduction of mean systolic blood pressure in the intervention group but elevated systolic blood pressure in non-intervention group. Both groups had improvement in diastolic blood pressure but the results were not significant within and between groups. The body mass index reduction was not significant in the intervention group but increased insignificantly in the non-intervention group and the difference between the groups was not significant.
There was a significant reduction of in mean total cholesterol in intervention group. Mean LDL cholesterol also reduced significantly. However, there were no significant changes in the TG and HDL cholesterol. New insulin cases were significantly higher in the intervention group as compared to the non-intervention group. Majority of the patients had addition of basal insulin.
CONCLUSION:
These findings provide evidence of the effectiveness of pharmaceutical care in diabetes and suggest that pharmacists shall expand their service, especially to patients with uncontrolled diabetes. The greatest improvements occur when pharmacists work in collaborative practice models. Growing evidence demonstrates that pharmacists, working as educators, consultants, or clinicians in partnership with other healthcare professionals, are able to contribute to improved patient outcomes.
How useful was this post?
- Benefits of outsourcing
- Benefits of outsourcing medical billing
- Customer service outsourcing India
- Customer support outsourcing
- Healthcare companies in the USA
- Healthcare outsourcing
- Healthcare outsourcing companies
- Healthcare outsourcing companies in India
- Healthcare outsourcing services
- It business process outsourcing
- It outsourcing company in India
- Medical billing
- Medical billing and coding outsourcing
- Medical billing outsourcing companies
- Medical billing services
- Medical coding
- Medical coding outsourcing
- Medical process outsourcing
- Outsource billing
- Outsource healthcare
- Outsource medical billing
- Outsource medical coding services
- Outsourced billing services
- Outsourcing
- Outsourcing companies
- Outsourcing companies in India
- Outsourcing Company
- Outsourcing in India
- Outsourcing medical billing to India
- Outsourcing medical services
- Outsourcing process
- Outsourcing providers
- Outsourcing service provider
- Outsourcing services
- Outsourcing services in India
- prior authorization
- Process outsourcing services
- Revenue cycle management outsourcing
- Revenue cycle outsourcing
Categories
Recently Posted
Tag Cloud
Build Your Team Today
Costs and improve efficiency!
Numbers Speak.
Tasks handled by our staff, updated in real-time.
Customer Service
Calls Handled
Prior Authorization
PAs Handled
Data Entry
Prescription Entries
Medical Billing
Bills/Claims Handled
Administrative
Tasks Handled











