Feb
A Review On Potential approaches towards Medical Coding Process in Clinical Data Management

Authors: – Miss.Pawar Kalyani G.1, Mrs.Deore Nisha N.2
Abstract
The basis of all countries information systems that Diagnose Related Groups to pay/finance hospitals is coded data. Both clinical and administrative data are included in this. It is essential to pinpoint the problems and barriers that affect the quality of coded data in order to enhance the data’s coding, usability, and outcomes. This article’s goal is to provide information about medical coding. In this essay, we’ll talk about how medical coders work inside health care and how COVID-19 has affected medical coding.
Introduction 1
Most individuals are not concerned about the staff employees who manage the paperwork after they see a doctor. Health plans and coders, on the other hand, play an important role in the background, assuring the correctness and up-to-datedness of customer records and bridging the divide between therapeutic practice and administration. Medical coding professionals are critical to the management and administration of health data and records in order to bill patients and collect reimbursement from insurance companies.
Medical coding is the act of translating a patient’s medical info into an alphanumeric character. Medical coders use their understanding of anatomy, medical terminology, illness, diagnostic techniques, and treatments to better understand the medical coding process. Information systems is not a subjective concept; rather, it is a specific system built on consolidated, standard texts that are recognized as the core of the health code. Examples include LMRP, ICD-10-CM, HCPCS Level II, and CPT.

Fig.01:- Introduction to Medical Coding. (Source-istock)
Medical Coding 2
Healthcare coding is the method of assigning conventional medical alphanumeric numbers to diagnoses, therapies, services, and devices used in healthcare. The information in the health records, such as the transcription of the doctor’s notes, the results of lab tests and radiologic exams, and so on, is utilized to generate diagnostic and procedure codes. Medical billing includes gathering the necessary information from supporting papers, assigning the proper codes, and filing a claim that will be reimbursed by insurance companies. Medical coding professionals help to ensure that the codes are applied appropriately during this operation.
Every time a patient sees a healthcare professional, medical coding is performed. Your doctor will go through your ailments and medical background, offer a professional diagnosis and treatment plan and document the appointment. Additionally, it keeps track of your payments to healthcare providers. Successful medical coding necessitates knowledge of biology, physiology, service specifics, payer laws and regulations, and the ability to read written music and operate an instrument to generate what is meant i.e. codes.
Need of Medical Coding
Documenting a clinical condition, test findings, and therapy is necessary for payment as well as to guarantee high-quality care during subsequent visits. The patient should be provided with understandable personal health information that stays with them throughout any following complaints and treatments. Given the tens of thousands of visits, treatments, and hospitalization that take in the United States every year, this is extremely crucial.
Functions of Medical Coders
The coder starts reading the medical notes or billing sheets at the beginning of the stack in order to comprehend the diagnosis given to the client and the procedures performed during the appointment. The coder also retrieves other crucial details from the paper, like the name of the treating physician, the date of the procedure, and other details.
Performing Medical Coding 3
Medical coders usually evaluate and code the patient records from the last day as the first task of the day. The type of records and notes will differ depending on the therapeutic environment (outpatient or institutional), and some degree of specialty may be required (the health care system may have individuals concentrated on health specialties; a wide range of patients and diseases for coders working in scale or more general clinics).
The coder starts reading the patient notes or invoicing sheets at the top of the stack in order to comprehend the diagnosis given to the patient and the procedures performed during the appointment. The coder also extracts other crucial details from the paper, like the name of the treating physician, the date of the procedure, and other details.
Coding is usually easy. Medical coders learn in-depth information about the procedures and patterns applied in a certain clinic or facility. Programmers may run upon challenging notes that demand in-depth investigation and careful coding. There are significant grey areas for developers to investigate even in the more widely used code. In extremely complicated or uncommon circumstances, interpreting coding requirements might be challenging. Expert programmers rely on their connections of peers and subject-matter experts to debate complexity in online forums, connect with subject-matter experts that meet at symposiums, consult with co-workers to solve challenges and enhance their code. Find a good problem to determine, or alternatively.
The encoder finally finishes the chart and starts the subsequent patient record. For every table, the process of reading, making notes, allocating codes, and entering information into a computer is repeated. The bulk of a programmer’s day is spent at a desktop reading notes, entering data into accountants, or searching for details to clarify papers.
Steps in the Medical Coding Process 3
- Document abstraction
Let me remind you that coder had to take anatomy and physiology (A&P) as well as medical terminology before enrolling in a coding class. Encourage them to have the A&P handbook and medical dictionary nearby so that they may check up any words or terminology that they don’t understand when reading the doctor’s notes. As an aspiring skilled programmer, it is critical to highlight the importance of using resources since precision is critical.
- Inquire as needed
Accuracy requires asking for further explanation or information, whether at work or in class. Questions and their responses pave the path for beneficial learning in the classroom and at work. Doctors’ documentation is egregiously deficient because they lack the knowledge that programmers require. And remember: It wouldn’t have occurred if it weren’t recorded. Ensure students that a code that is unknown does not require reporting. Queries enhance the document with all required detail to achieve coding precision.
- Code Diagnosis or Diagnosis
- Code procedure
Courses often concentrate on diagnosis or coding techniques, but the fundamentals stay the same. Determine the most precise and explicit code to mirror documentation. Encourage pupils to use resources so that they have the accurate understanding of the material.
- Confirmation of medical necessity
The next step a qualified medical coder takes is to match diagnostic and procedure codes to support a medical necessity. It’s possible that you’ll need to consult your A&P texts, but being rational and critical thinking is generally helpful. Mention websites like Nlm [found high levels], the online medical dictionary and encyclopedia of the American Medical Association and the Institutes Of health to students as well.
- Check the coding
Give your pupils a few minutes to code backward (review the code, read the directions again, and contrast with the documentation). Tell yourselves that it’s always preferable to make amends for your errors.
On the market, there are several standardized medical coding dictionaries. The five dictionaries that are stated below are utilized for encoding, however.
- COSTART – Side effect term thesaurus code symbols.
- ICD9CM – International Classification of Diseases 9 Revision Clinical Correction.
- MedDRA – Medical Dictionary of Regulatory Activities.
- WHO-ART – World Health Organization Terminology for Adverse Reactions.
- WHO-DDE – Enhancing the World Health Organization’s Drug Dictionary.
Above the five dictionaries are listed, MedDRA and the WHO are two that are often used to categorize medical terminology used in clinical trials. The global Drug Index of the World Health Organization (WHODRUG) This dictionary is regularly updated and maintained.
A report from the University Monitoring Center (UMC). The most extensive dictionary with medication information is this one.
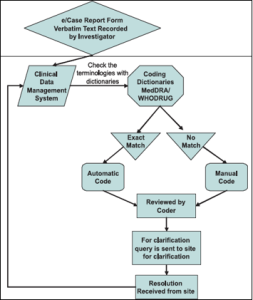
Fig.02:- Flow Chart of Medical Coding Process. 4
Fig.03:- Process Chart of Medical Coders
In order to pay the bill, the insurance company must understand what happened after a medical professional examined or treated the patient. Since a basic fundamental is too vague to provide insurance companies with the precise information they want, a specialized set of characters has been devised to designate medical operations. Medical coding is a technical language used in the medical and commercial industries. A physician coder is an expert who translates physicians and other medical professionals notes into a standardized set of codes that insurance companies may utilize.
Impact of COVID-19 on Medical Coding 7
The medical coding method has been altered as a result of the COVID-19 outbreak.
Prevalence of electronic claim administration in the medical and dentistry industries, for example, grew by 2.3% in 2020. These interactions include qualifying and benefit assessment, pre-approval, claim reporting, claim status inquiry, claim payment, and reference confirmation in the healthcare business. With the development of the new virus, medical claims and programmers have had to establish new codes and return processes.
In March 2020, WHO assigned the first COVID-19 ICD-10 code. Since then, at least 12 new ICD procedure codes for the virus have been created, while CPT and HCPCS codes have undergone several adjustments to better represent COVID-19 and related disorders.
During the pandemic, CMS also made major modifications to its Medicare physician fee schedule, which impacted medical billing systems and programmers. The new recommendations urge clinicians to evaluate and manage (E/M) indicates that the code can be picked, rather than depending on a patient’s physical examination and medical history to decide the right E/M code.
Healthcare and coding are crucial components of the medical value chain. By maintaining the seamless operation of billing and coding cycle, providers get paid for their services and provider organizations stay accessible to serve patients.
Conclusion
The translation of operations, medical exams, medical services, and gadgets into medical numerical form is known as medical coding. Reducing and correcting health coding and billing errors has a significant influence on a company’s accuracy and bottom line. The most prevalent issues were poor documentation, inaccurate code and modifiers, service opening up, and a lack of understanding of coding concepts, anatomy, and medical terminology. Medical coder mistakes can be reduced with appropriate training in coding rules, monitoring and auditing medical language, comparative anatomy, medical symbols, and diagnostics. Coding and billing mistakes may be avoided, but understanding why they occur will help decrease and manage them.
According to the Journal of Medical Systems, the worldwide economy for internal medicine, which is predicted to be valued $15.2 billion in 2019, will increase at a CAGR of 9.6 percentage points over the following five years (2020–2030).
References:-
[1] A Review on Medical Coding & Billing Errors and its Management, Jyothi M Borkar, Manjunatha R, International Journal of Science and Research (IJSR) ISSN: 2319-7064, SJIF (2019): 7.583
[2] https://www.aapc.com/medical-coding/medical-coding.aspx
[3] Shelley Safina, 6 Key Steps in the Medical Coding Process, December 4, 2019 https://www.mheducation.com
[4] Babre D. Medical Coding in Clinical Trials. Perspect clin res 2010; 1; 29-32
[5] Ashfaque Aatqb, Johar. (2019). What Exactly Is Medical Coding?
[6] CIGMA – medical coding academy https://www.cigmahealthcare.in
[7] Evcycle intelligence xtelligent healthcare media, June 15, 2018.
https://revcycleintelligence.com.
[8] Academy of Medical Coders India https://igmpiindia.org.
How useful was this post?
- Benefits of outsourcing
- Benefits of outsourcing medical billing
- Customer service outsourcing India
- Customer support outsourcing
- Healthcare companies in the USA
- Healthcare outsourcing
- Healthcare outsourcing companies
- Healthcare outsourcing companies in India
- Healthcare outsourcing services
- It business process outsourcing
- It outsourcing company in India
- Medical billing
- Medical billing and coding outsourcing
- Medical billing outsourcing companies
- Medical billing services
- Medical coding
- Medical coding outsourcing
- Medical process outsourcing
- Outsource billing
- Outsource healthcare
- Outsource medical billing
- Outsource medical coding services
- Outsourced billing services
- Outsourcing
- Outsourcing companies
- Outsourcing companies in India
- Outsourcing Company
- Outsourcing in India
- Outsourcing medical billing to India
- Outsourcing medical services
- Outsourcing process
- Outsourcing providers
- Outsourcing service provider
- Outsourcing services
- Outsourcing services in India
- prior authorization
- Process outsourcing services
- Revenue cycle management outsourcing
- Revenue cycle outsourcing
Categories
Recently Posted
Tag Cloud
Build Your Team Today
Costs and improve efficiency!
Numbers Speak.
Tasks handled by our staff, updated in real-time.
Customer Service
Calls Handled
Prior Authorization
PAs Handled
Data Entry
Prescription Entries
Medical Billing
Bills/Claims Handled
Administrative
Tasks Handled











